This study [1] aimed to examine tissue changes in patients with head and neck squamous cell carcinoma (HNSCC) after primary radiochemotherapy (RCT) using radiomic feature analysis. Patients with locally advanced HNSCC frequently require primary RCT. Despite intensity modulation, the desired radiation-induced effects observed in HNSCC may also be observed as side effects in healthy tissue, e.g., the sternocleidomastoid muscle (SCM). The optimal time window for salvage surgery, a treatment often considered after primary RCT, is generally believed to be between 6 to 12 weeks post-RCT. This timeframe is largely determined by clinical studies focusing on surgical complications, rather than directly exploring radiation's impact on the SCM.
This study is the first to explore short-term RCT-induced skeletal muscle alterations after RCT in HNSCC patients applying radiomics, a data-driven approach aiming at extracting and processing quantitative data to analyze image-based information
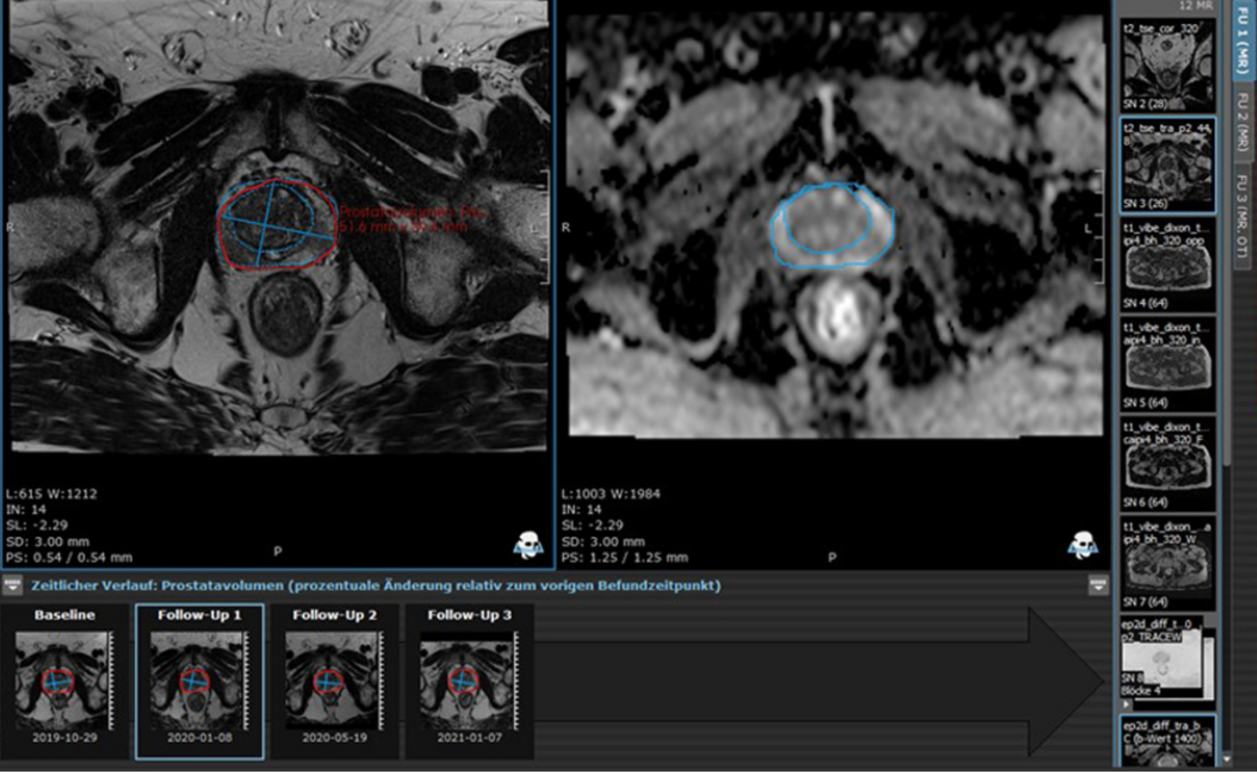
Using the mint Lesion™ Radiomics module, researchers analyzed the CT scans of 98 HNSCC patients, focusing on three key radiomic parameters: volume, mean positivity of pixels (MPP), and uniformity.
The study revealed a significant reduction in volume after primary RCT. Specifically, the SCM volume decreased from 9.0 to 8.4 mL, and the paravertebral musculature (PVM) volume dropped from 96.5 to 91.9 mL. This observed decrease was unexpected, as an increase was anticipated due to inflammation and edema in the SCM directly affected by irradiation. Moreover, a significant drop in PVM volumes was noted, which was primarily influenced by chemotherapy and not irradiation.
It was determined that these volume changes were unlikely to be caused solely by irradiation, chemotherapy, or their combination. In the course of the study, significant reductions were observed in both BMI (from 23.9 to 21.0 kg/m²) and serum protein levels (from 7.4 to 6.6 mg/%). These observed reductions were found to be closely correlated with the changes in volume. Once the results were adjusted for the variations in BMI, the volume changes for SCM and PVM post-treatment were rendered insignificant.
The findings of this study underscore the paramount importance of closely monitoring and optimizing patients' nutrition before, during, and after undergoing primary RCT. Previous studies have linked lower serum protein levels and BMI to increased complication rates in patients who later undergo salvage surgery. When accounting for changes in BMI, no significant alterations in muscle volume or other radiomic features indicative of tissue fibrosis were found. Thus, this study supports the existing clinical consensus that the best period for salvage surgery following RCT lies between 6 to 12 weeks.
Read the original publication here.
[1] Santer, M.; Riechelmann, H.; Hofauer, B.; Schmutzhard, J.; Freysinger, W.; Runge, A.; Gottfried, T.M.; Zelger, P.; Widmann, G.; Kranebitter, H.; et al. Radiomic Assessment of Radiation-Induced Alterations of Skeletal Muscle Composition in Head and Neck Squamous Cell Carcinoma within the Currently Clinically Defined Optimal Time Window for Salvage Surgery—A Pilot Study. Cancers 2023