Early MRI scans are critical for patients who have just undergone brain tumor resection to evaluate the surgery's success and plan future treatments. However, the presence of intracranial air often creates "artifacts" or visual distortions that make these scans difficult to read.
In a recent study, Christer Ruff et al. evaluate a more robust imaging technique to solve this problem.
The Challenge: Postoperative Imaging Obstacles
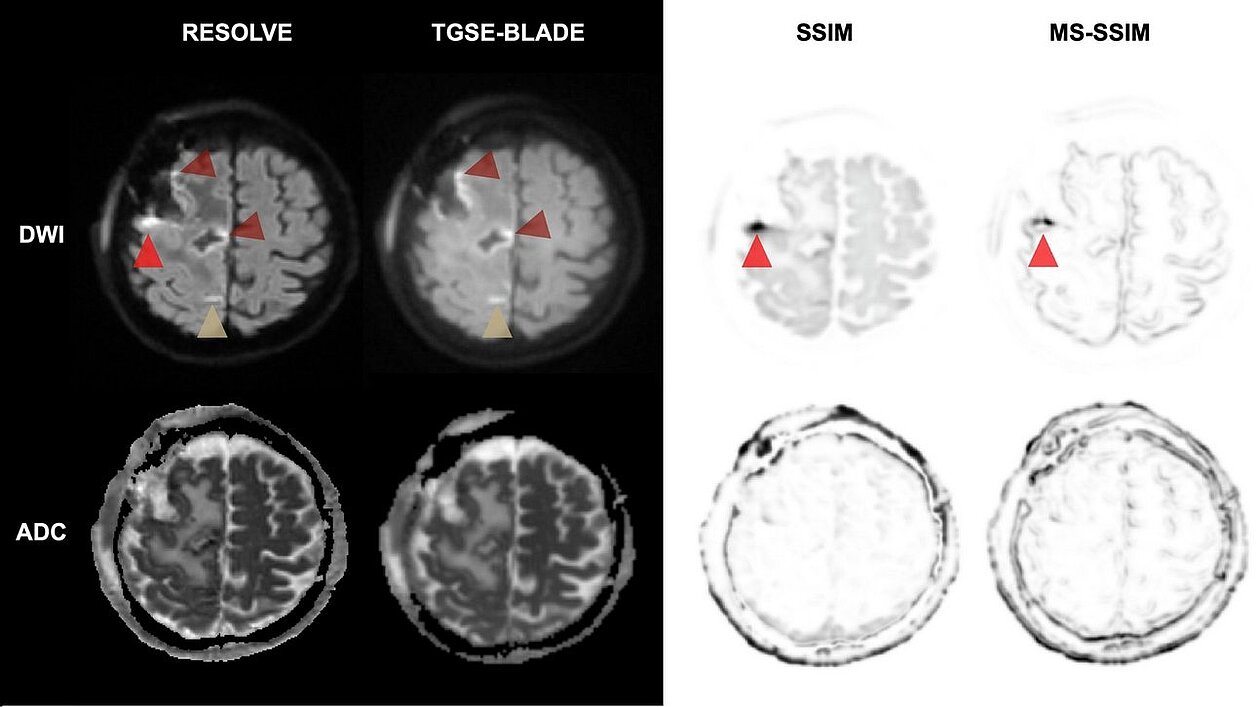
Diffusion-weighted imaging (DWI) is essential for identifying perioperative ischemic changes (minor strokes or tissue damage) near the resection site. Standard techniques like RESOLVE DWI are often impaired by geometric distortions and susceptibility artifacts caused by air-tissue interfaces after surgery. The presence of these distortions complicates the distinction between artifacts, ischemic changes, and postoperative alterations, making it challenging to obtain a clear diagnostic image.
The Study: Comparing TGSE-BLADE and RESOLVE
Researchers conducted a retrospective study of 33 patients who underwent 1.5-Tesla MRI within 48 hours of brain tumor resection. The study compared two advanced techniques:
- RESOLVE DWI: A common technique that segments data to reduce some distortion.
- TGSE-BLADE DWI: A non-EPI technique using a "radial" data acquisition strategy designed to be insensitive to magnetic field inhomogeneities.
mint Lesion, a software solution for a standardized and computer-assisted review of imaging and clinical data, was used to perform bidimensional measurements of the resection defect across different imaging sequences.
By comparing these measurements to standard T1-weighted reference images, the team could objectively quantify which DWI technique provided the most accurate, distortion-free view of the surgical site.
Key Outcomes and Findings
The study found that TGSE-BLADE DWI outperformed RESOLVE in several critical areas:
- Reduced Distortion: TGSE-BLADE showed significantly fewer geometric distortions and artifacts near the resection site compared to RESOLVE (p < 0.001).
- Higher Accuracy: Measurements of the resection area on TGSE-BLADE images closely matched the T1-weighted reference scans, whereas RESOLVE showed significant discrepancies due to image warping.
- Diagnostic Confidence: Neuroradiologists reported significantly higher diagnostic confidence and better overall image quality when using TGSE-BLADE.
- Trade-offs: While RESOLVE DWI provided a slightly higher signal-to-noise ratio (SNR), the clarity and lack of distortion in TGSE-BLADE made it the superior tool for clinical assessment.
Conclusion: A Possible New Standard for Postoperative Care
The study concludes that TGSE-BLADE DWI is a robust alternative to conventional sequences for postoperative brain imaging. By minimizing artifacts caused by intracranial air, it allows doctors to clearly distinguish between expected post-surgical changes and actual ischemic brain damage. This leads to more accurate follow-up assessments and improved long-term patient care.
Read the original publication here.
Christer Ruff, Till-Karsten Hauser, Paula Bombach, Daniel Vogl, Constantin Roder, Frank Paulsen, Deborah Staber, Vivien Richter, Leonie Zerweck, Ulrike Ernemann, Georg Gohla. “A comprehensive quantitative and qualitative assessment of TGSE-BLADE DWI in postoperative imaging following intracranial tumor resection.” European Journal of Radiology, Volume 196, 2026, ttps://doi.org/10.1016/j.ejrad.2026.112659.