
Lung Cancer Screening in Germany – A Turning Point for Early Detection
Few topics are currently as impactful in radiology as lung cancer screening. From 2026, Germany is expected to roll out a nationwide program, marking a milestone in prevention, but also introducing significant challenges for clinical practice.
Lung cancer remains one of the most common and deadliest cancers worldwide. Early diagnosis is critical to improving survival rates [1]. The official launch of a national lung cancer screening program for high-risk individuals could be a watershed moment for early detection. But what does this mean for the healthcare system—and especially for radiology?
Lung Cancer Screening in Germany
On June 18, 2025, Germany’s Federal Joint Committee (G‑BA) approved a lung cancer screening program for heavy smokers aged 50–75. This decision builds on the new Lung Cancer Early Detection Regulation (LuFrühErkV).
Key details of the screening program:
- Target group: Active and former smokers aged 50–75
- Method: Low-dose CT (LDCT)
- Eligibility: Insured individuals with at least 25 pack-years history, either current smokers or those who quit within the past 10 years
- Process: Structured eligibility assessment, standardized imaging, and dual readings for suspicious findings
- Implementation: Scheduled for April 2026, pending final approval from the Federal Ministry of Health
This initiative marks a major advance in lung cancer early detection in Germany [2], presenting a timely opportunity to support radiologists with high-quality solutions.
What Lung Cancer Screening Means for Radiologists
The new lung cancer screening program further strengthens the central role of radiologists, not just in early cancer detection, but also in standardized reporting, risk assessment, and patient follow-up [3].
They will face significantly higher demands, including mandatory advanced training and certification specific to lung cancer screening [4]. A corresponding increase in CT scans will bring greater workload and time pressure [5], particularly with longitudinal patient monitoring. Additionally, the ongoing integration of updated or newly published guidelines (such as those from ESTI and Lung-RADS) will become a challenge in daily practice.
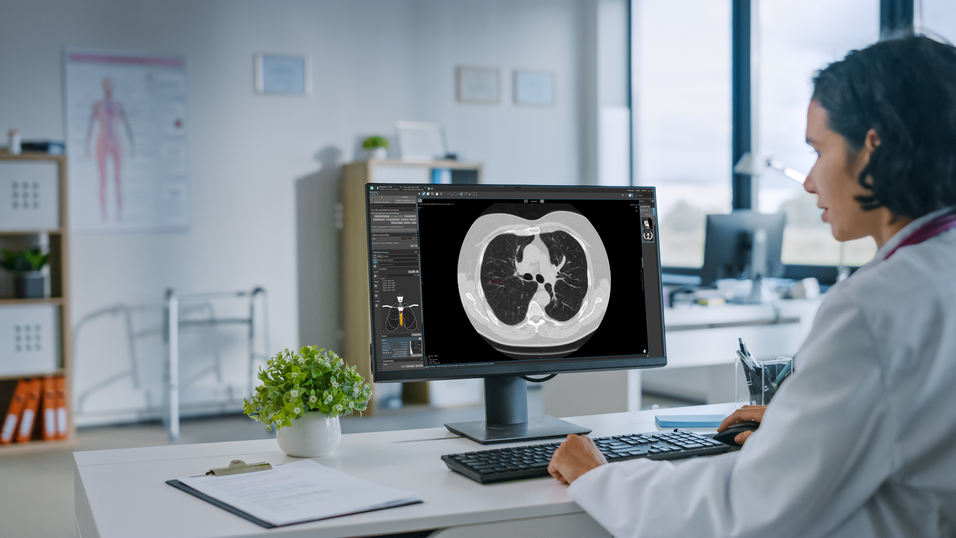
How Mint Medical Can Support You
Innovative tools like mint Lesion are designed to help radiologists meet these challenges by:
- Automating nodule detection
- Enabling standardized, structured reporting aligned with evolving guidelines
- Integrating into existing workflows
- Supporting follow-up management with AI-based insights
Our Contribution to the Future of Early Detection
At Mint Medical, we understand that the future of lung cancer screening relies not just on early detection, but also on the efficient management of patient data. mint Lesion facilitates both AI-powered detection and guideline-based workflow management—two pillars essential for successful screening programs.
Benefits of mint Lesion for lung nodule management
- AI-assisted nodule detection
Powered by ADVANCE Chest CT by contextflow - a leading AI tool for lung CT analysis. Detected nodules are flagged as provisional findings and can be confirmed with a single click; segmentation can be adjusted directly in the image. - Structured reporting
Complete reporting is done within the platform, ensuring consistency and structure. - Workflow integration
mint Lesion integrates into existing radiology practices. - Clinical decision support for nodule management
mint Lesion helps radiologists deliver precise, guideline-compliant diagnoses and make confident treatment decisions. - Automated risk assessment & guideline compliance
Recommendations for nodule management are generated automatically according to national or institutional guidelines. Tools like Lung-RADS, volume-doubling time (VDT) and the Brock cancer-risk model are built in, and updates are added promptly so you are always aligned with current standards.
Why It Matters
With the screening program scheduled for rollout in 2026, the outlook for early lung cancer detection in Germany is promising. We are closely monitoring developments and continuously updating mint Lesion to reflect the latest guidelines and best practices. Our mission is to deliver innovative solutions that help radiologists ensure accurate, timely, and comprehensive patient care.
Contact us for a live demo of mint Lesion or to find out how we can support you in navigating this new era.
Sources
[1] World Health Organization. 2025. „Cancer.“ World Health Organization, 03.02.2025. https://www.who.int/news-room/fact-sheets/detail/cancer.
[2] Federal Joint Committee. 2025. „Lungenkrebs-Früherkennung bei starken Raucherinnen und Rauchern wird voraussichtlich ab April 2026 Kassenleistung.“ Gemeinsamer Bundesausschuss, 18.06.2025. https://www.g-ba.de/presse/pressemitteilungen-meldungen/1263/#:~:text=Das%20Screening%2D%E2%80%8BAngebot%20kann,und%20auch%20die%20Versicherteninformation%20vorliegt.
[3] Snoeckx, Annemiek, Franck, Caro, Silva, Mario et al. 2021. “The radiologist’s role in lung cancer screening.” Translational Lung Cancer Research 10.5: 2356-2367. http://dx.doi.org/10.21037/tlcr-20-924.
[4] Aunt Minnie Europe. 2025. „Lung cancer screening receives green light in Germany.” Aunt Minnie, 23.06.2025. https://www.auntminnieeurope.com/clinical-news/ct/news/15749108/lung-cancer-screening-receives-green-light-in-germany.
[5] Harder, Jan Niklas and Maßberg, Joachim Felix. 2022. „Acceptance of AI technology for lung cancer screening diagnosis.” Department of Informatics, Lund School of Economics and Management, Lund University. https://lup.lub.lu.se/luur/download?func=downloadFile&recordOId=9081588&fileOId=9081592
Related Resources
Successful “RECIST and Beyond” Workshop in Cologne: Advancing Precision in Oncologic Imaging
How can complex tumor findings be assessed accurately, reproducibly, and in line with clinical guidelines?
Implementing RANO 2.0 for Neuro-Oncology Clinical Trials in mint Lesion
Tumor response assessment in neuro-oncology clinical trials requires careful attention to measurement protocols and confirmation scan requirements. To…
RACOON – Imaging, Data & Collaboration for Better Decisions
Modern radiology faces a central question: how can imaging and clinical data be combined in a way that leads to more precise diagnoses,…